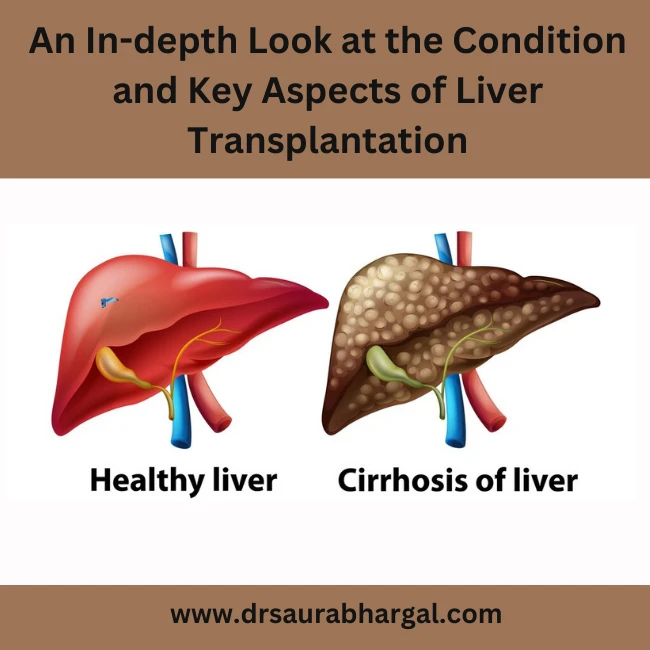
Cirrhosis is a progressive and potentially life-threatening condition that affects the liver. It occurs when healthy liver tissue is gradually replaced by scar tissue, leading to impaired liver function. In severe cases, liver transplantation becomes a crucial consideration for those with advanced cirrhosis. In this guest post, we will delve into the nature of cirrhosis, its causes, symptoms, and when the option of a liver transplant should be considered.
Table of Contents
ToggleUnderstanding Cirrhosis
Cirrhosis develops over a long period, often as a result of chronic liver diseases like hepatitis C, hepatitis B, fatty liver disease, or excessive alcohol consumption. As the liver tries to heal itself from repeated damage, scar tissue accumulates, hindering its ability to function efficiently. As the condition progresses, the liver’s capacity to filter toxins, produce essential proteins, and regulate various bodily functions diminishes.
Signs and Symptoms of Cirrhosis
Early stages of cirrhosis might not manifest noticeable symptoms, making early detection and intervention crucial. As cirrhosis advances, individuals may experience fatigue, easy bruising, jaundice (yellowing of the skin and eyes), swollen abdomen and legs due to fluid retention, itchy skin, and confusion. These symptoms indicate that the liver’s function has been significantly compromised and that medical attention is necessary.
When to Consider a Liver Transplant
Liver transplantation is considered a viable option when cirrhosis reaches an advanced stage where the liver’s ability to function has been severely compromised, and other treatments are no longer effective. The decision to undergo a liver transplant is not taken lightly, and a comprehensive evaluation by a medical team is crucial.
Several factors contribute to the decision-making process for a liver transplant:
Severity of Cirrhosis:
Transplant candidacy is determined based on the severity of cirrhosis, often assessed using scoring systems like the Model for End-Stage Liver Disease (MELD) or Child-Pugh score. These systems consider factors like bilirubin levels, creatinine levels, and prothrombin time.
Liver Function:
A deteriorating liver function despite medical management can indicate the need for a transplant. As cirrhosis progresses, the liver’s ability to perform vital functions, such as detoxification and protein synthesis, becomes severely compromised.
Quality of Life:
If cirrhosis symptoms significantly impact an individual’s quality of life, a transplant may be considered to improve their overall well-being.
Complications:
The development of severe complications like hepatic encephalopathy (confusion and altered mental state due to liver dysfunction) or refractory ascites (fluid buildup in the abdomen) can prompt the need for a liver transplant.
Response to Treatment:
If the cirrhosis is caused by a treatable underlying condition, a liver transplant may be considered if other treatment options have failed.
Conclusion
Cirrhosis is a serious condition that requires careful management and timely intervention. Liver transplantation is a life-saving option for those with advanced cirrhosis, where the liver’s function is critically compromised, and other treatments have proven ineffective. Early detection, proper medical care, and lifestyle changes can help delay or even prevent the progression of cirrhosis.
It’s essential for individuals at risk of cirrhosis, such as those with chronic liver diseases or a history of excessive alcohol consumption, to undergo regular medical check-ups and follow their healthcare provider’s recommendations.
If you or a loved one are facing the possibility of a liver transplant due to cirrhosis, seeking guidance from a qualified medical team is imperative. Decisions regarding liver transplantation are complex and require a comprehensive assessment of an individual’s medical history, current condition, and overall well-being. Remember, medical advancements continue to improve the outcomes of liver transplantation, offering hope and a chance at a healthier life for those affected by advanced cirrhosis.